SU2C Canada PASS Convergence Dream Team
Team Leaders: Jennifer J. Knox, MD, Elizabeth M. Jaffee, MD
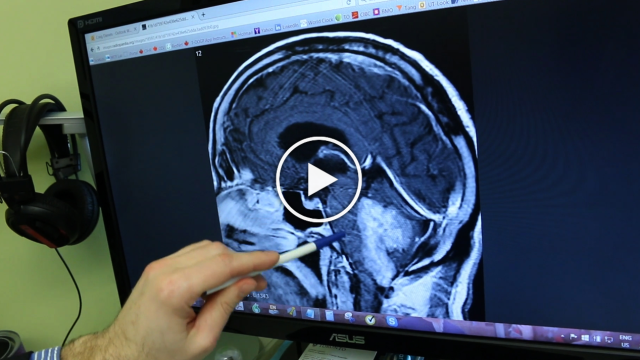
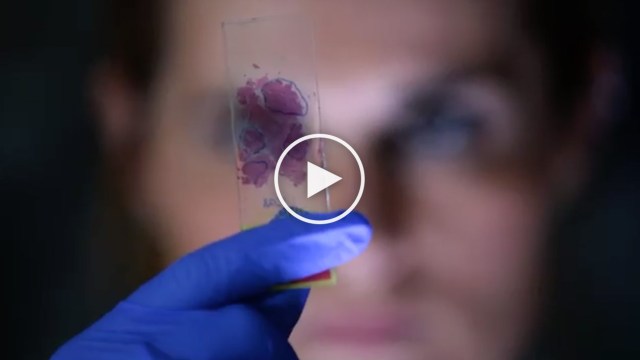
This Dream Team is testing ways to use the molecular characteristics of the tumor to predict which medicines should be prescribed preferentially and develop tests to distinguish specific tumor sub-types. This team is carrying out a randomized phase II clinical trial of FOLFIRINOX compared to gemcitabine/ nab-paclitaxel as first line treatment in metastatic pancreatic ductal adenocarcinoma.
SU2C Canada Metastatic Breast Cancer Dream Team
Team Leaders: Nahum Sonenberg, PhD Michael Pollak, MD
This Dream Team is investigating a new way to treat metastatic breast cancer by interrupting the ability of breast cancer cells to manufacture the proteins they need to aggressively spread to organs beyond the breast. The new treatment, being tested for the first time in humans, strikes at the process that allows breast cancer to go from a localized problem to a potentially fatal disease. If successful, this work will open a new approach to the treatment of metastatic breast cancer.
Scientific Abstract (PDF)
Team Progress Updates (PDF)
“We are going after the process in which the genetic code is translated into proteins. In cancer, this process can go wrong and promote metastasis. We have drugs that we think can keep this process from working and thereby prevent metastasis.”—Nahum Sonenberg, PhD, McGill University
SU2C Canada Cancer Stem Cell Dream Team
Team Leaders: Peter Dirks, MD, PhD Samuel Weiss, PhD
The SU2C Canada Cancer Stem Cell Dream Team’s goal is to understand the abnormalities in cancer stem cells found in brain tumors, specifically glioblastomas in adults and children and posterior fossa ependymomas in infants. Team members are working to find vulnerabilities in these cells, to identify new drugs that may be effective against them, and to test these drugs in preclinical mouse models.
Scientific Abstract (PDF)
Team Progress Updates (PDF)
“Our team will conduct multiple analyses of brain cancer stem cells, profiling their biological makeup to identify drugs that are likely to block the uncontrolled growth of the tumors, and carry out clinical trials across Canada to find the safest and most effective drugs to treat these cancers.”—Peter B. Dirks, MD, PhD, Hospital for Sick Children
SU2C Canada–Canadian Cancer Society Breast Cancer Dream Team
Team Leaders: Tak W. Mak, PhD Samuel Aparicio, PhD
The SU2C Canada–Canadian Cancer Society (CCS) Breast Cancer Dream Team has accelerated the research and development of three new drugs intended to treat aggressive forms of breast cancer. The Dream Team’s approach, called targeted therapy, has been to identify and make use of characteristics in the cancer cells that distinguish them from normal body cells.
Scientific Abstract (PDF)
Team Progress Updates (PDF)
“We will give our new drugs to patients for whom other treatments have not worked, and monitor them to see whether a significant percentage of these patients responds to one or more of these drugs. By respond, we mean that we hope these patients’ tumours shrink, or at least that their disease holds steady rather than getting worse.”—Tak W. Mak, Campbell Family Institute for Breast Cancer Research at Princess Margaret Cancer Centre